
Many unpredictable, devastating events happened as we entered the year 2020. An awakening outbreak of a respiratory illness caused by a new virus emerged in Wuhan City, Hubei Province of China.
Public health experts worldwide are scrambling to detect, track, and contain this new coronavirus that appeared in Wuhan, China, toward the beginning of December 2019.
The World Health Organization alerted several cases of pneumonia in the area, but the virus did not match previous coronaviruses, such as SARS and MERS.
What Are Coronaviruses?
Coronavirus is named for its shape, protruding spikes that look like a crown or ”corona.” SARS and MERS are part of the coronavirus and viruses that cause the common cold.
They are zoonotic, meaning they spread between animals and people. The zoonotic family includes many viruses that cause the common cold and more severe respiratory illnesses.
Animal Source of this Coronavirus
It isn't clear what animal the virus originated from. However, one investigation found that the hereditary arrangement of the new virus is 96 percent similar to that of a coronavirus found in bats. Both SARS and MERS started with bats.
How It Was Transmitted From Animals To Humans
Coronaviruses are a large group of viruses that occur in animals. These viruses mutated, making it possible for them to infect humans. Like their relative coronaviruses, coronaviruses attack the respiratory system. Now, they have caused fatalities and overwhelmed healthcare providers around the world.
What Is Covid-19

COVID-19 is a contagious disease caused by the most recently identified coronavirus. This new virus and infection were unfamiliar before the outbreak started in Wuhan, China, in December 2019. COVID-19 is currently a pandemic affecting several nations worldwide.
A case was examined, examining early instances of the illness. Published on January 24th, it found that the first patient to become ill didn't contact the market. Specialists are still attempting to trace the outbreak to its source.
An Emerging Outbreak In China
The World Health Organization named the illness brought about by the COVID-19 infection. The name hints at the type of infection and the year it surfaced.
At least 106 people have died from a new coronavirus in China following an outbreak in the central city of Wuhan. It forced the government to lock down nearly 20 cities. In effect, it has quarantined an estimated 56 million people.
Updated reports show more than 18 million confirmed cases have been recorded globally. There are more than 700,000 deaths.
Many are in China, particularly Wuhan and the neighboring cities in Hubei province. However, the rate of new cases there has slowed down. Almost 12 million individuals have recovered from the ailment, which affects 213 countries and territories worldwide.
Spreading Outside China

Most new cases are appearing in nations other than China. There have been huge disease outbreaks in South Korea, Italy, Iran, and Japan. By the end of January 2020, the World Health Organization (WHO) declared a world public health emergency.
The virus has spread to over 200 countries and regions in three months. The first coronavirus case outside China was in Thailand in mid-January, and the first recorded death outside China was in the Philippines by the beginning of February. These signs pushed several leaders worldwide to order travel bans and declare “lockdown” or quarantine periods.
World Cases Of COVID-19
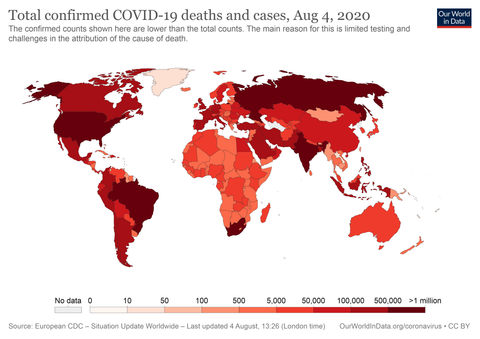
There have been 18,709,161 cases of COVID-19 worldwide, with at least 704,000 deaths in 213 countries and territories. The World Health Organization website provides information for each country. The Americas have the most confirmed cases, with 9,741,727. Europe came second with 3,425,017 instances.
As of August 4th, the United States has the most cases globally, almost 5 million. Brazil now came in second, amounting to over 2 million cases. Countries such as India, Russia, and South Africa came in next.
Surprisingly, the countries mentioned above surpassed the number of cases where the disease's epicenter is. China now recorded 84,491 confirmed cases and came 29th in the most number of cases.
The United States also has the highest number of deaths, with over 160,000. Brazil came second, more than half of what the US has recorded, with 96,000 deaths. You can visit the latest metrics of COVID-19 cases worldwide here.
China has entered a new phase in the COVID-19 outbreak: suppression. China has driven coronavirus transmission to almost zero, although few new cases have been reported.
Still, nearly all of them were imported cases of travelers who recently returned from abroad.
Where And How It Originated
At the end of December, public health authorities from China informed the World Health Organization about an issue. They said an unknown, new virus was causing pneumonia-like ailment in Wuhan. They immediately discovered that it was a coronavirus. And that it was quickly spreading through and outside of Wuhan.
Origin of the Virus
Chinese health specialists are yet trying to determine the starting point of the virus. They stated it originated from a seafood market in Wuhan where wildlife was traded illegally. This seafood market is called the Huanan Seafood Wholesale Market.
The WHO additionally says an animal source appears to be the primary source of the outbreak.
How It Is Transmitted
Chinese health specialists have indicated that the new coronavirus can be transmitted from person to person. The virus is also evolving, which may allow it to spread more rapidly and complicate treatment.
It isn't yet clear how infectious the virus is. Many other coronaviruses are notorious for spreading through coughing and sneezing, but there are no signs that the virus is transmitted through the respiratory tract.
Incubation Period
The COVID-19 virus is thought to have a 14-day incubation period. The median time from exposure to the onset of symptoms is 4-5 days. A study showed that 97.5% of persons with COVID-19 developed symptoms 11.5 days after the infection.
Person-to-person Spread
The virus is thought to spread mainly from person to person.
-
Between people in close contact (within about 6 feet).
-
Respiratory droplets are produced when an infected person coughs, sneezes, or talks.
-
These droplets can land in the mouths or noses of nearby people or who can inhale them into the lungs.
-
Some recent studies suggested that COVID-19 may spread to people not showing symptoms.
-
Maintaining a reasonable social distance (about 6 feet) is critical in preventing the spread of COVID-19.
“Can Covid-19 be caught from a person who has no symptoms?”
COVID-19 is spread through respiratory droplets. These droplets are discharged by somebody who is coughing or has different manifestations. Examples of these are fever or sleepiness. Numerous individuals with COVID-19 experience just mild symptoms.
This is especially evident in the beginning periods of the infection. It is likely to get COVID-19 from somebody who has only a mild cough and doesn't feel sick.
A few reports showed that individuals without symptoms could transmit the virus. It isn't yet known how frequently this occurs. WHO is evaluating continuous examination on the topic and will continue to share updated data.

Asymptomatic Instances
Several cases have already been reported of patients who are COVID-19 positive but never developed symptoms (asymptomatic). These asymptomatic people are not routinely tested, so their infection and detection are poorly understood.
Chinese authorities have said that they have seen situations where individuals with the virus infected others before they began showing symptoms. Research from China indicated that individuals without symptoms have significant virus levels in their throats and noses. This means they might pass the virus if they cough or sneeze.
In one study, confirmed cases in children were asymptomatic using reverse-transcriptase-polymerase chain reaction (RT-PCR). Patients may have abnormalities on chest imaging before showing symptoms.
Asymptomatic Transmission
Many epidemiologic studies have documented COVID-19 transmission during the incubation period. This time is called the “pre-symptomatic” incubation period. Studies have shown large quantities of viral RNA and viable viruses from asymptomatic and pre-symptomatic persons.
It is unclear how viral RNA shedding and transmission of COVID-19 are related. It is also unclear how transmission due to asymptomatic or pre-symptomatic infection compares to symptomatic transmission.
The Symptoms of Covid-19

According to the WHO, the signs and symptoms of COVID-19 vary on the onset of the illness. But most persons infected with the virus would experience the following:
Fever CoughShortness of breath Breathing difficultiesMuscle or body achesFatigueLoss of taste or smell sore throat runny or congested noseDiarrhea
The symptoms vary according to the severity of the disease. For example, cough, fever, and shortness of breath are more familiar to hospitalized with COVID-19 than those with mild cases (non-hospitalized patients).
Statistics and Presentation of Symptoms in the World
80% of people recover from the infection without requiring hospital treatment. Around 1 out of 5 individuals who get COVID-19 turn out to be actively sick and develop trouble breathing.
In one study, 44% of the 1,099 patients admitted to the hospital had fever, which increased to 82% during hospitalization. Headache, fatigue, and muscle aches (myalgia) are the most commonly reported hospitalization symptoms. Nasal congestion, runny nose, and sore throat are also distinguishable symptoms.
Many COVID-19 patients experience gastrointestinal symptoms such as vomiting, nausea, or diarrhea. They sometimes experience these signs and symptoms before developing fever and lower respiratory tract symptoms.
Loss of smell or taste is mainly reported in women and young or middle-aged COVID-19 patients. These patients showed these symptoms before experiencing respiratory symptoms, although they did not need hospitalization.
Although many COVID-19 symptoms are common to other respiratory or viral illnesses, loss of smell appears more specific to COVID-19.
Some older adults and persons with medical comorbidities-a situation when one experiences two medical conditions at the same time would later experience fever and respiratory symptoms.
It can prompt pneumonia, severe acute respiratory disorder, kidney failure, and even death in increasingly severe cases. Elderly citizens tend to be more often affected by the virus than younger people.
Children show the same signs and symptoms as adults but vary by the child's age. However, they have milder cases compared to adults.
The severity of the Infection

According to the persons infected with COVID-19 in China, the severity of the illness can range from the following:
- Mild to moderate (mild symptoms up to mild pneumonia): 81%
- Severe (dyspnea, hypoxia, or >50% lung involvement on imaging): 14%
- Critical (respiratory failure, shock, or multiorgan system dysfunction): 5%
The deaths that occurred among patients with critical illness have an overall fatality rate of 2.3%. Patients with the critical disease have a fatality rate of 49%.
In China, children have an illness severity lower than 49% for asymptomatic, mild, or moderate disease. 5% of them have severe disease. Less than 1% have the critical disease.
In the US, 19% of COVID-19 cases with known dispositions were hospitalized. The proportion of those admitted to the intensive care unit (ICU) was 6%.
Progression of the Severity
The average time from the onset of illness or symptoms ranged from 5 to 8 days for severe (dyspnea) case patients. The average time from the onset of symptoms ranged from 8 to 12 days for patients with acute respiratory distress syndrome (ARDS). Lastly, the average time from the onset of illness or symptoms to ICU admission ranged from 10-12 days.
Clinicians need to be aware of the potential for some patients who could deteriorate rapidly in a week after the onset of the illness. Among hospitalized patients, 26%-32% were admitted to ICU. Among all patients, 3% to 17% developed ARDS compared to 20% to 42% for hospitalized patients. 67% to 85% of patients were admitted to ICU.
Mortality rates of patients admitted to ICU were 39% to 72%. This range depends on the study and characteristics of the patient population. The average length of days for hospitalized survivors was 10 to 13 days.
Risk Factors for Severe Infection
Age is a strong risk factor for severe infection, complications, and even death. In the majority of the confirmed cases in China alone, the case fatality rate was highest among ages more than 80 years old.
In China, Here are the case fatality rates among other age groups:
- Above 89 years old----14.8%
- 70-79 years old ----8%
- 60-69 years old ----3.6%
- 50-59 years old ----1.3%
- 40-49 years old ----0.4%
- Less than 40 years old---0.2%
In US epidemiological data, the following are the case fatality rates:
- 85 years and above-----10%–27%
- 65-84 years----3%–11%
- 55-64 years---1%–3%
- 55 years and less------ <1%
In China, reports also showed as low as 0.9% fatality rates for patients with no underlying medical conditions. However, it had the highest rates for patients with comorbidities. These medical conditions include cardiovascular disease, diabetes, chronic respiratory disease, or cancer.
Stroke, diabetes, chronic lung disease, and chronic kidney disease have also been linked with increased severity of the COVID-19 infection.
It is also important to note that patients with heart disease are at a higher risk for COVID-19 infection.
Mortality results were consistent in China and the US, accounting for the age differences and prevalence of underlying conditions in COVID-19 patients.
Reinfection
No data accounts for the possibility of reinfection with COVID-19 after recovery. The viral RNA may shed but continue for days or weeks during recovery. However, detecting this viral RNA during testing may not indicate that the viruses are viable to infect.
When the body becomes infected with COVID-19, it creates IgM and IgG antibodies. However, clinical studies don’t have definitive data, and it is uncertain whether the presence of these antibodies can protect against possible reinfection.
Also, the results didn’t show how much concentration of these antibodies is enough for the protection.
Another Covid-19 Variant
Most recent headlines about the ongoing COVID-19 pandemic are alarming: Another variant of the virus is currently rising in the United States.
How many variants are out there?
Why the delta variant is alarming
How delta variant symptoms are different
- Fever or chills.
- Cough.
- Shortness of breath or difficulty breathing.
- Fatigue.
- Muscle or body aches.
- Headache.
- New loss of taste or smell.
- Sore throat.
- Congestion or runny nose.
- Nausea or vomiting.
- Diarrhea.
- Coughing.
- Sneezing.
- Runny nose.
- Upset stomach.
- Headache
- Fatigue.
What do we know about other COVID variants?
What about the lambda variant?
Does the vaccine protect against variants?
When To Seek Medical Help?
If you develop the emergency warning signs for COVID-19, get medical attention immediately. These emergency warning signs are:
- Persistent pain or pressure in the chest
- Trouble breathing
- New confusion or inability to arouse
- Bluish face or lips
However, if you live in an area with dengue fever or malaria, it is significant that you don't disregard fever symptoms. Look for clinical assistance. When you go to the health office, wear a mask as much as possible, keep an excellent 1-meter distance from others, and don't contact surfaces with your hands. If a child is sick, aid the child and adhere to this guidance.
Remember that these may not show all at once. Seek your medical provider for any other severe symptoms.
Who Should Be Tested?

Not everyone should be tested for COVID-19. The CDC provides guidance on who should be tested. However, decisions about testing are at the discretion of state and local health departments and individual clinicians.
Here are the criteria for priority patients with suspected COVID-19 infection:
Priority 1
- Hospitalized patients
- Healthcare facility workers with symptoms
Priority 2
- Patients in long-term care facilities with symptoms
- Patients 65 years of age and older with symptoms
- Patients with underlying conditions with symptoms
- First responders with symptoms
Priority 3
- Critical infrastructure workers with symptoms
- Individuals who do not meet any of the above categories with symptoms
- Healthcare facility workers and first responders
- Individuals with mild symptoms in communities experiencing high numbers of COVID-19 hospitalizations
Non-priority
- Individuals without symptoms
Different COVID-19 Tests
Molecular (Swab) Test

Healthcare workers use a swab test to take specimens from the nose and back of the throat of PUIs. Each sample is then put in a tube, sealed, and taken to the national or subnational confirmatory testing laboratory for COVID-19.
Once the samples arrive in a qualified testing facility, technicians use rRT-PCR or real-time reverse transcriptase-polymerase chain reaction. This is to look for novel coronavirus or severe acute respiratory syndrome coronavirus 2.
Although the results may be negative, there is still a high index of suspicion for COVID-19 virus infection. This was mainly the case when only upper respiratory tract specimens were collected. A re-examination is necessary. Additional specimens, including the lower respiratory tract, should be collected and tested.
Antibody (Serology) Test

This type is a blood test. It detects the presence of antibodies that help fight against the coronavirus. The particular types are immunoglobulins IgM and IgG. They are specific to this type of infection.
Depending on the clotting factors, these antibodies are in the liquid part of the blood, called serum or plasma. Their presence may be detected separately or together.
Here are signs you should take this test:
- You are a health worker exposed to the virus and experienced common signs and symptoms.
- You traveled or lived in a place where there is a local transmission of COVID-19.
- You are living or have close contact with a suspected or confirmed case of COVID-19.
- You have recovered from COVID-19
IgM Antibody Test
This test detects the IgM antibodies that first form when a virus attacks. A positive IgM test indicates that you have recently been infected. Thus, your immune system responds quickly by producing them. A test showing IgM positive means you may still be infected. Or it could be that you just recently recovered from a COVID-19 infection.
IgG Antibody Test
This test detects the IgG antibodies that develop in patients within seven to 10 days after the symptoms. These antibodies remain in the blood after the infection. The result would indicate that you may have had COVID-19 in the recent past. These antibodies that develop may protect you from future infection. Still, no data shows how long these antibodies can protect from reinfection.
What Can Be Done to Stop It From Spreading
There is no specific treatment for the new virus. Yet, many studies are in progress that attempt to discover a few. One driving applicant is remdesivir, an antiviral medicine initially created to treat Ebola. Clinical preliminaries are testing it in patients in China and the US.
Research groups and pharmaceutical organizations are also attempting to develop a vaccine that could potentially protect individuals from the disease. However, vaccine advancement takes a long time. Whether everything goes quickly or not, it will be around a year to 18 months and a half before one is accessible.
State media reported that Chinese authorities have effectively closed Wuhan. Airports worldwide, especially in China, have introduced fever checks for travelers from China.
Since the outbreak has been declared, this calls for a worldwide public health emergency. Restrictions for international travel, tighter border checks, and setting up special treatment centers and quarantine areas have been intensely practiced.
How To Protect Yourself From The Disease

Good hygiene is strongly recommended to prevent this virus from spreading. Follow these simple reminders from the Centers for Disease Control and Prevention.
- Wash your hands often with soap and water for at least 20 seconds. If soap and water are not available, use an alcohol-based hand sanitizer.
- Avoid touching your eyes, nose, and mouth with unwashed hands.
- Avoid close contact with people who are sick.
- Stay home when you are sick.
- Cover your cough or sneeze with a tissue, then throw the tissue in the trash.
- Clean and disinfect frequently touched objects and surfaces.
- Strengthen your immune system by eating fruits and vegetables
- Drink plenty of water
If you live in the US, you almost certainly have the flu or the common cold. It's still flu season. Elevated levels of flu action aren't relied upon to subside at any point shortly. (It's not very late to get a flu shot!)
Call your doctor if you live in the US and have a fever or a dry cough. Do so if you have recently been to China, Iran, Italy, Japan, or South Korea. Have a check-up when you have been in contact with somebody who has been to one of those spots or been in contact with somebody who has a confirmed case of COVID-19.
Can a face mask protect you from infection?
The CDC suggests that people not vaccinated wear cloth face masks when they go out in the open. They should also wear one if they are at home with someone infected or exposed.
A mask is an additional layer of protection for everybody, on top of social distancing efforts. You can spread the infection when you talk or cough, regardless of whether you don't realize that you have it or, on the other hand, in case you're not showing symptoms.
The CDC urges that surgical masks and N95 masks ought to be reserved for healthcare workers and front liners.
Is it safe to travel during a pandemic?
There is a higher chance of getting COVID-19 in crowded places. The CDC advises opposing international or cruise ship travel during the pandemic. Restrictions are being facilitated for the vaccinated individuals, and a few regions are using "vaccine passports" to open up to vaccinated travelers.
Below are a couple of questions that might help you with concluding whether it's safe to travel:
- Is the Covid spreading where you're going?
- Will you have close contact with others during the trip?
- Is it accurate to say you are in greater danger of serious illness if you contract the infection?
- Do you live with somebody who has a serious medical condition?
- Will where you stay be cleaned?
- Will you have access to food and different necessities?
If you’ve decided to travel, avoid sick people. Wash your hands regularly and try not to touch your face.
Wear a face mask when you are around others. All airlines require all passengers to wear them. Face masks are also needed for different types of public transportation, such as trains and buses.
Treatment
There is neither a specific medication to treat nor a vaccine to prevent COVID-19. Since this is a viral infection, antibiotics are not suggested. Treatment available is only for the symptoms. Oxygen therapy represents the first step in helping people cope with respiratory impairment. Intensive care will help deal with complicated forms of the disease.
Research laboratories around the world are testing different possible treatments for the disease. However, supportive care may be given to relieve symptoms, which include:
- Pain relievers (acetaminophen or ibuprofen)
- Cough syrup or medication
- Rest
- Fluid Intake
There is supportive care for patients experiencing shortness of breath or a respiratory rate of less than 28-30/min. Administration of oxygen by a 40% Venturi mask is necessary for them.
“Is a Vaccine, Drug or Treatment Available for Covid-19?”

According to the World Health Organization, no specific vaccines or medicines for COVID-19. However, laboratories and companies worldwide compete to procure vaccines and drugs, which are still under investigation and undergoing clinical trials.
For some Westerners, conventional or home remedies may give comfort and lessen symptoms of mild COVID-19.
WHO doesn't suggest self-medication with prescriptions, including antibiotics, to prevent or remedy COVID-19. Instead, it is organizing a resolution to create vaccines and drugs to prevent and treat COVID-19 and will continue to provide updated data as soon as research results become available.
Treatments Under Investigation: A Case Study
Remdesivir has been proven to shorten the recovery time for hospital patients. However, it does not work for everyone who receives it.
A team of scientists, including Sumit Chanda, a Sanford Burnham Prebys Medical Discovery Institute professor, has identified 21 existing drugs that can stop the replication of SARS-CoV-2, the virus that causes COVID-19.
The team performed extensive testing and validation studies, including evaluating the drugs on human lung biopsies infected with the virus. They also evaluated the drugs for synergies with remdesivir and established dose-response relationships between them and their antiviral activity.
Of the 21 drugs that were effective at blocking viral replication, the scientists found the following:
- Thirteen of them could potentially be safely achieved in COVID-19 patients. They have reached clinical trials before.
- Two are already FDA-approved: astemizole and clofazimine.
- Four worked synergistically, including an antimalarial drug reaching the Phase 3 trial.
The team is currently pursuing 21 compounds in small animals. "Based on our current analysis, clofazimine, hanfangchin A, apilimod, and ONO 5334 represent the best near-term options for an effective COVID-19 treatment," says Chanda.
"While some of these drugs are currently in clinical trials for COVID-19, we believe it's important to pursue additional drug candidates, so we have multiple therapeutic options if SARS-CoV-2 becomes drug-resistant."
Vaccine
Scientific research around the world is growing to develop a SARS-CoV-2 vaccine. There are more than 100 candidates for vaccines in development. If those, 8-10 are under clinical investigation.
Chinese researchers appear to be in the lead in procuring a vaccine. Nevertheless, several studies are also ongoing in the US and the UK.
On Dec. 11, 2020, the FDA granted an emergency use authorization (EUA) in the U.S. for the Pfizer-BioNTech COVID-19 vaccine. Within seven days, that organization also granted an EUA to a vaccine developed by Moderna. Johnson and Johnson's single-shot vaccine was granted an EUA in February 2021.
The British government supported and started to give the Pfizer vaccine on Dec. 8, 2020. Vaccines created in China and Russia are likewise being given in several countries.
The Pfizer and Moderna vaccines require two doses, taken half a month apart, while J and J are only a single shot.
Healthcare workers and the elderly were initially given priority in getting the vaccines; however, by May 2021, the vaccines were made accessible to anybody over 12 years old.
These vaccines were developed uncommonly fast, with testing in people beginning in March 2020. The FDA says no corners were cut to consider endorsement and that the vaccinations are safe.
The CDC has said they are alright for pregnant women, and there's no proof that antibodies shaped by the COVID-19 vaccination cause any issues with pregnancy.
Prevention
The best approaches to protect yourself as well as other people against COVID-19 are to:
- Clean your hands as often as possible and thoroughly
- Refrain from contacting your eyes, mouth, and nose
- Cover your cough with the bend of the elbow or tissue. If a tissue is used, dispose of it immediately and wash your hands.
- Keep up a distance of at least 1 meter from others.
Difference Between Self-isolation, Self-quarantine, and Social Distancing
Self-quarantine implies limiting activities or isolating individuals who are not sick but may have been exposed to COVID-19. The objective is to prevent the spread of the virus when individuals may be asymptomatic.
Self-isolation implies separating individuals who are sick with symptoms of COVID-19. This is also for those who might be infectious to prevent the spread of the illness.
Social distancing implies being physically separated from others. WHO suggests keeping a good 1-meter distance from others. This is a general measure that everybody should take, regardless of whether they are well and have no known exposure to COVID-19.
How Is China Trying To Stop The Virus?

China made a forceful move toward the outbreak's beginning. It closed down transportation in Wuhan, home to more than 11 million individuals, and canceled flights and trains in and out of the city.
Many cities were put under successful quarantine to slow the spread of the infection to other nations. Many festivities for the Lunar New Year, a gigantic holiday in China, were not spared from cancellation.
China likewise suspended public social events. They isolated the sick individuals and forcefully followed their contacts. They also had a devoted system of clinics to test for the virus.
The number of new infections announced in China has been declining. This showed WHO authorities that transmission was easing back down, indicating that their control measures were working.
Coronavirus Updates In The United States
There have been 2,388,153 confirmed cases and 122,610 deaths in all 50 states in the US. In the United States, you can check the latest update on COVID-19 here. You can also see the latest updates here in each state.
The growing number of lab-confirmed cases in the US is still behind. This cannot be compared to the seasonal flu, which kills an estimated 12,000 to 16,000 annually. Experts say these respiratory diseases are similar to severe pneumonia. What’s worse is that they don’t have any treatment.
History of COVID-19 in the United States
Jan. 21, 2020: First confirmed case in the US
A man in his 30s from Washington State with a travel history to Wuhan has been diagnosed with the novel coronavirus.
Jan. 31, 2020: Coronavirus a public health emergency
On Jan.31, 2020, the United States declared Coronavirus a Public Health Emergency. It issued a 14-day quarantine rule for US citizens entering the US from China. It also issued an order to deny entry to foreigners in China within the past two weeks.
Feb. 26, 2020: First case of Suspected Local Transmission in the United States
On Feb. 26, 2020, it recorded the first suspected local transmission in the United States. The Centers for Disease Control and Prevention (CDC) confirms the first case of COVID-19 in a patient in California. This patient did not have any travel history in an outbreak area nor contact with a COVID-19 patient. Soon, Washington, Oregon, and New York reported their first cases of possible community transmission.
Feb. 29, 2020: First death reported in the United States
On Feb. 29, 2020, the United States reported its first death from COVID-19 in Washington state. It was a man who had no travel history to China. But, there were already two deaths that occurred last Feb. 26 at a nearby nursing home. This would later become the first COVID-19 death in the United States.
Mar. 13, 2020: US President Trump declares a national emergency
President Donald Trump declared the U.S. national emergency. He said it would open up $50 billion in federal funding to fight COVID-19.
Mar. 17, 2020: Coronavirus now present in all 50 states
West Virginia was the last state to have no cases and has reported its first case. It also means that the disease is present in all 50 states. North California ordered “shelter in place” for six counties in the San Francisco area for three weeks. It means people are to remain in their homes. They are to follow it unless they leave their house for important reasons or exercise outdoors.
Mar. 20, 2020: New York City declared as US outbreak epicenter
New York City reported more than 15,000 positive cases of COVID-19, accounting for almost half of the infections in the US. Mayor Bill de Blasio warned that the outbreak would worsen as supplies declined.
Mar. 26, 2020: US leads the world in COVID-19 cases
The United States now has the most number of confirmed cases in the world. It recorded cases topping 82,000 and deaths topping 1,000.
Mar. 27, 2020: $2 trillion stimulus bill signed by Trump
This $2 trillion coronavirus relief law guarantees loans to small businesses and creates a lending system for distressed companies. It also gives financial assistance to hospitals that are frontlines of the crisis.
Apr. 9, 2020: Evidence showed the first coronavirus case in NYC came from Europe
A new study has found evidence that the first COVID-19 cases in New York City originated in Europe. It occurred as early as February. Researchers found that COVID-19 in NYC arose in an untracked transmission between the United States and Europe. This evidence is limited. But, it has supporting evidence showing direct introductions from China, where the virus originated.
April 21, 2020: Autopsy stirs up a positive note as 1st US COVID-19 death was earlier than previously suspected
The CDC affirms that tissue from a person in Santa County, California, who passed away on Feb. 6, tested positive for COVID-19. That passing happened weeks sooner than the COVID-19 deaths in the Seattle region on Feb. 26. It was already believed to be the country's first.
May 27, 2020: US reaches 100,000 deaths
The pandemic has now killed more than 355,000 people worldwide and more than 100,000 people in the United States.
June 11-17, 2020: Cases in Arizona, South Carolina and Florida soar
States that rushed to reopen their economies saw subsequent increases in COVID-19 cases, hospitalizations, and deaths.
June 24, 2020: NY, NJ, Conn. tell Florida travelers to quarantine
As the United States outbreak shifts from the Northeast to the South and West, several states restrict travelers from Florida.
July 12, 2020: Florida breaks single-day record for new COVID-19 cases
Florida reports 15,000 new COVID-19 cases daily, surpassing New York's one-day record of 12,000 in April.
Aug. 7, 2020: COVID-19 outbreak at Georgia summer camp infects 260
A CDC report finds that two hundred sixty campers and staffers tested positive for COVID-19 at a youth sleepaway camp in Georgia, with 76% of those tested receiving positive results.
Sept. 22, 2020: US reaches 200,000 deaths
The pandemic has now killed more than 965,000 people worldwide and more than 200,000 people in the United States.
September 23, 2020: A new, more contagious strain of COVID-19 is discovered
A study conducted at Houston Methodist Hospital finds a more contagious strain of COVID-19 in a large portion of recent patient samples. Experts analyzed samples from the earliest phase of the pandemic and a more recent infection wave, finding that nearly all strains from the more recent phase had a mutation that allows the virus to bind and infect more cells.
October 9, 2020: US signs deal with AstraZeneca
The Trump administration signed a $486 million agreement with AstraZeneca to develop an antibody treatment for COVID-19.
October 22, 2020: FDA approves Remdesivir as first COVID-19 drug
Gilead’s remdesivir is the first FDA-approved drug to treat COVID-19 after three randomized trials found it to decrease the length of hospital stays and reduce the likelihood that patients will require oxygen.
November 4, 2020: US reports unprecedented 100,000 cases in 1 day
The US hits a grim milestone with 100,000 new COVID-19 cases reported in a single day for the first time.
November 9, 2020: President-elect Biden announces COVID-19 transition team; Pfizer publishes vaccine results
After former Vice President Joe Biden was determined to be the president-elect on November 7, he announced the names of the scientific, medical, and public health professionals who will serve on his Transition COVID-19 Advisory Board. The same day, Pfizer released data from its COVID-19 vaccine trial showing that the vaccination was 90% effective.
November 16, 2020: Moderna reveals vaccine efficacy results
The positive vaccine news continues with Moderna’s announcement that its experimental vaccine reduces the risk of COVID-19 infection by 94.5% in participants who received it.
December 10, 2020: FDA advisory panel recommends Pfizer, BioNTech COVID-19 vaccine
An FDA advisory panel endorses the first COVID-19 vaccine. The application for the Pfizer and BioNTech vaccine was discussed during a lengthy public meeting. Voting 17-4, with one abstention, the Vaccines and Related Biological Products Advisory Committee (VRBPAC) decided that the vaccine's benefits outweigh its risks for people 16 and older.
December 18.2020: FDA signs off on EUA for Moderna's COVID-19 vaccine
The FDA issued the second EUA, allowing the shipment of the Moderna COVID-19 vaccine to begin.
December 23, 2020: US buys more Pfizer vaccine
The Trump administration announced buying 100 million doses of Pfizer and BioNTech’s vaccine.
December 31, 2020: US falls short of goal to give 20 million vaccinations by year ed
As the year closed, the CDC says about 2.8 million people have received an initial vaccination. The US said on December 30 that about 14 million doses have been distributed out of 20 million allocated doses.
How At-Risk Is The United States?
It's difficult to state how noteworthy an impact it could have in the United States. However, the virus is spreading throughout the nation. The CDC uses its guidelines for the pandemic flu as a beginning stage for preparation.
Individuals in the US ought to get ready for disturbances to regular daily life, said Nancy Messonnier. She is the National Center for Immunization and Respiratory Diseases executive at the CDC during a press call.

There are more than 400 confirmed instances of the virus in the US, including individuals who were diagnosed with COVID-19 and need to evacuate.
The US State Department ordered it from Wuhan and the Diamond Princess cruise ship, which is set to undergo quarantine in the US. Nineteen individuals in the United States have died of the virus. A progressing episode is occurring at a nursing home in Washington state.
There are cases in states including California, New York, Washington, Oregon, and Florida in individuals who didn't contact someone known to be contaminated with COVID-19. The source of those diseases is unknown. This might mean the infection is spreading through communities in the United States. The infection may have been spreading in Washington for quite a long time.
Accordingly, the CDC rules initially didn't permit testing except if a sick individual had been in a nation with a continuous infection spread or had been in contact with somebody with an affirmed case of the disease. These people could be tested but postponed the diagnosis of patients who didn't have those risk factors.
Since then, the information has been updated to state that doctors can use their best judgment based on a patient's symptoms and area of concern. The choice to be tested depends on the patient's choice. In the US, however, there is still a limited number of accessible tests.
The CDC likewise says that it intends to conduct widespread examinations for the infection. This is to check whether there are missing issues in testing units that eased back in the beginning. Inclining that up is significant because different nations are looking to discover them.
Moreover, any foreign national who has traveled to China in the previous 14 days will not be permitted to enter the US. However, President Trump declared that they were exempt if they had close relatives there. The WHO doesn't support that choice. It said nations should not limit travel or exchange their reactions to the virus.
Above all, it is essential to be extra cautious about our health. As the most cliché line says, “Prevention is better than cure.”
← Older Post Newer Post →





